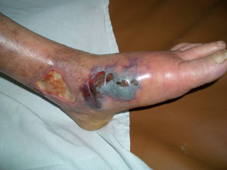
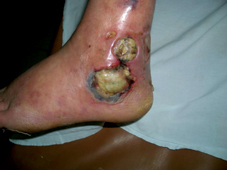
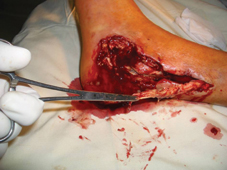
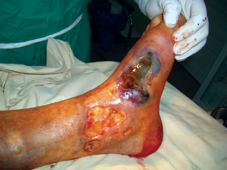
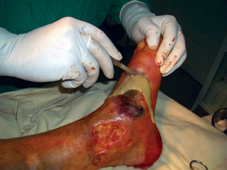
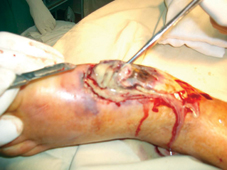
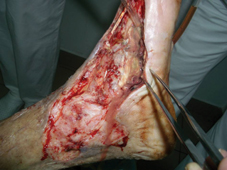
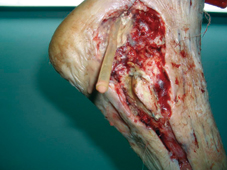
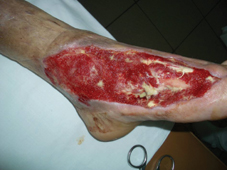
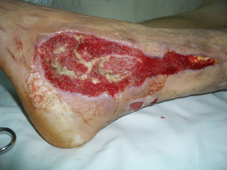
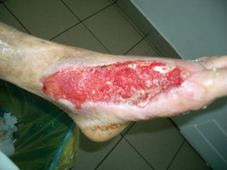
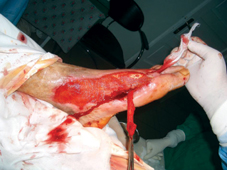
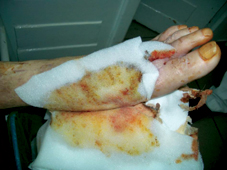
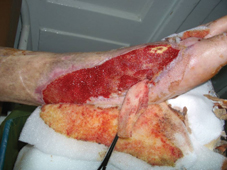
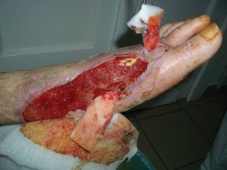
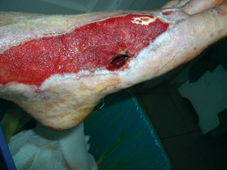
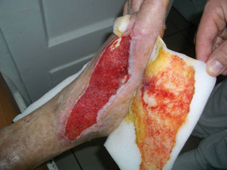
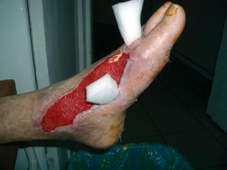
60 years old female patient, with neglected leg ulcers, who developed a necrotic cellulitis of the left foot and ankle.
Fig. 19: Finally shorter pieces of LIGASANO® are inserted in the first web space and the plantar space (without crossing between these two spaces), because the new granulation tissue filled the deep tunnel created by sepsis and sloughing. This case is still in process and the granulation area has to be grafted.